CLAUDICATION
 Claudication is used to describe the crampy pain in patients legs with peripheral arterial disease. It often develops after walking a certain distance. The pain usually resolves with rest and is predictable. Patients tend to have this pain after walking a certain distance and they adjust their lives accordingly. The pain can be severe but it will go away after resting just a few minutes.
Claudication is used to describe the crampy pain in patients legs with peripheral arterial disease. It often develops after walking a certain distance. The pain usually resolves with rest and is predictable. Patients tend to have this pain after walking a certain distance and they adjust their lives accordingly. The pain can be severe but it will go away after resting just a few minutes.
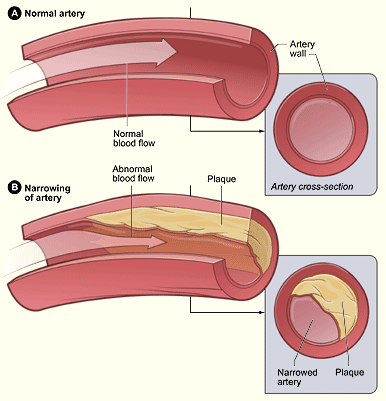
Claudication happens because the arteries of the leg are so narrow that when the leg needs more blood for exercise, there just isn’t a wide enough passage for blood to go through. This causes a shortage of blood delivery which is painful. In most cases, patients don’t have pain without activity. When they walk, more blood is required to deliver oxygen to the tissues. Their narrowed vessels are unable to deliver the required blood flow and pain ensues. This is claudication. When activity stops, blood is again delivered in adequate amounts to the tissues and the pain goes away.
Causes and risks
Claudication is a symptom of peripheral arterial disease (PAD) which is caused by atherosclerosis. Therefore, the factors which increase the risk for atherosclerosis are the same as those which increase the risk for claudication.
Risk factors for atherosclerosis include:
- Smoking
- High cholesterol levels in the blood
- High blood pressure
- Obesity
- Having a family history of heart or vascular disease
Diagnosis
One of the most important ways to diagnose claudication is with a good history and physical exam. Other types of pain can mimic claudication, so it can sometimes take an experienced vascular surgeon to determine whether or not claudication is indeed present.
After an exam, if we suspect PAD and claudication, a surgeon may order other tests such as:
- Ankle-brachial index (ABI) which compares the blood pressure in the arms and legs.
- Pulse volume recording which measures the volume of blood at various points in the legs.
- Duplex ultrasound which shows blood flow in the vessels in the leg, and can detect the location and number of specific narrowings.
- Blood tests for cholesterol, high blood sugar, or other markers for artery disease.
- Magnetic resonance angiography (MRA), which is an advanced MRI which can show the blood vessels in the legs.
- Computerized tomographic angiography (CTA), which is an advanced CT scan which can generate pictures of your blood vessels in 3D.
- Angiography – a more invasive procedure where the arteries are injected with dye and pictures are obtained.
Treatment
PAD is a very serious condition because it indicates that significant atherosclerosis is present in the body. Remember, atherosclerosis is the condition that most often leads to serious and deadly conditions like heart attacks and stroke!
Therefore, we take PAD very seriously and work with patients to strictly control their risk factors for atherosclerotic disease. We aggressively treat high blood pressure, diabetes, and high cholesterol. We help you with a real plan for regular exercise and a healthy diet, often referring you to a dietician when needed. If you are a smoker, we work with you to stop smoking at all costs. When appropriate, we test you for other conditions, such as aortic aneurysms, carotid artery disease, and heart disease, so we discover these conditions and treat them before they become dangerous. We add medications which are known to be beneficial in patients with PAD, such as aspirin and plavix in certain patients.
Conservative treatements
Claudication, surprisingly, is not always treated with surgery. In fact, only a minority of patients with claudication will require any procedures. Most patients can avoid surgery by doing two things: Regular exercise (5 times weekly, walking to the point of pain, then resuming once the pain dissipates), and smoking cessation. But of course, this can be harder than it looks! Many patients inquire if compression stockings are a viable treatment for claudication. They are not. Compression stockings may actually worsen the condition by impeding blood flow.
Medication
It is a vascular surgeon’s job to make sure that patients with claudication are managed medically by treating high blood pressure, diabetes, high cholesterol, and encouraging patients to maintain a healthy weight. We also typically start platelet inhibitors, like aspirin, or Plavix, because this is beneficial in patients with claudication. We also make sure typically that the patient has a cardiologist, because the presence of claudication indicates atherosclerotic disease, which is often found also in the heart, and can be very dangerous. This way, a whole team of doctors helps each patient minimize risk of atherosclerosis and live their healthiest lives.
Surgery
If the claudication persists, then there are obviously options for treatment, usually in the form of minimally invasive procedures, but this is only required in about 10 percent of people with claudication. Procedures usually requires general anesthesia and usually involves a few days in the hospital. For certain patients, this is the best option to treat claudication.
