Deep Vein Thrombosis (DVT) – Blood Clot
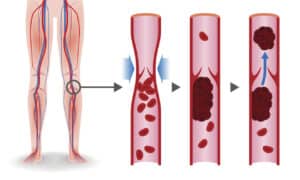 Deep vein thrombosis (DVT) is when a blood clot (thrombosis) develops in the deep veins of the leg. People susceptible to DVT are those who have been sedentary or have had injury. Deep vein thrombosis is dangerous because a blood clot can break off from its location and travel through veins to other parts of the body causing serious and sometimes fatal damage to the heart or lungs. Learn more about DVT, its prevention, and its treatment.
Deep vein thrombosis (DVT) is when a blood clot (thrombosis) develops in the deep veins of the leg. People susceptible to DVT are those who have been sedentary or have had injury. Deep vein thrombosis is dangerous because a blood clot can break off from its location and travel through veins to other parts of the body causing serious and sometimes fatal damage to the heart or lungs. Learn more about DVT, its prevention, and its treatment.
Risks for DVT – Blood clot in leg
Patients who are at risk for blood clots (DVT) are those who:
- have been sitting or lying down for prolonged periods of time without moving – like those who have been on a long airplane or car ride or someone who is bedridden.
- have venous insufficiency or damaged veins
- have a condition where their blood is prone to clots – sometimes associated with a blood disorder, cancer, or extreme dehydration.
- have had recent surgery – especially orthopedic surgery to the hip or knee.
- have had trauma like a pelvic injury or a broken leg.
- have a spinal injury and paralysis.
Dangers of DVT
A DVT is dangerous because blood clots that develop in the legs can break off and float to other parts of the body where it can effect both the heart and lungs. Blood flows from veins travels into the right side of the heart and out to the lungs where it picks up oxygen. It returns to the heart and is pumped back out into the body to deliver oxygen. If blood clots float into the lungs and become stuck it is called a “pulmonary embolism” or PE. and can be very dangerous – even fatal.
DVT can also damage the veins in the leg – especially if the clot is extensive. In this case, the damaged veins can be serious because the deep venous system is large and responsible for bringing most of the blood back up to the heart against gravity. If these deep veins are blocked with a blood clot, the clot can injure the valves over time leading to an ineffective venous system. Patients then may have debilitating swelling and severe venous insufficiency in their leg which leads to skin changes and ulcers. They can also have severe pain called post-phlebitic syndrome. It is a dreaded complication of extensive DVT that can occur even with adequate anticoagulation therapy. If the clot is extensive or if blood thinner treatment is not possible, patients can be referred to a vascular surgeon for further evaluation and possible surgical treatment.
DVT symptoms
A deep vein thromboses blood clot is most often found when there is leg swelling that involves only one leg. It usually develops over a day or two and can be painful. If questioned, the patient can usually think of something that put him or her at risk like a long plane ride or recent surgery. Some of the most common symptoms of DVT are:
- Swelling and tightness of the leg
- A cramp-like feeling in the leg
- Pain while walking
- Red discoloration around the painful area
- Warm skin around the painful area
DVT Diagnosis
If you suspect DVT, you should be diagnosed as soon as possible. Your vein doctor should start by asking a series of questions to determine if DVD is likely. If your doctor suspects a DVT, he or she will immediately obtain an ultrasound. The ultrasound allows the doctor to see blood flow in the venous system and determine if there is a blockage or clot. It is imperative that the ultrasound be completed as soon as possible. There are also other tests that the clinician may use to diagnose DVT such as a D-dimmer test and contrast venography.
DVT treatment
If the ultrasound results show a clot in the leg, DVT treatment with blood thinners are started immediately. Your doctor will explain these medications to you. They must be taken and monitored very carefully. The blood thinners are very important because they allow the body to break down the blood clot slowly over time and they are effective at preventing the clot from floating into the lungs (pulmonary embolism).
