VENOUS DISORDERS & VENOUS INSUFFICIENCY
What is venous insufficiency?
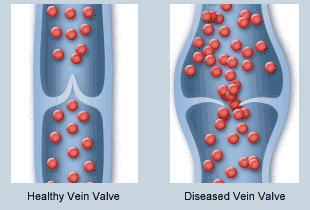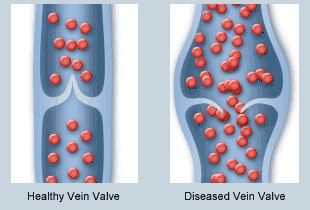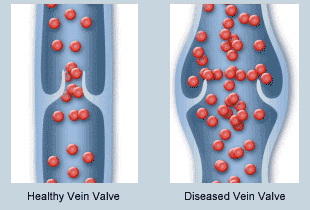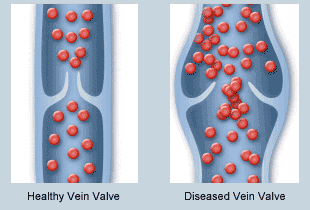
Healthy veins have one-way valves that help pump blood efficiently back up to the heart. Damaged or weakened valves become insufficient and can no longer prevent blood from flowing backward and pooling in the veins. This increases the pressure in the affected veins and over time additional damage occurs from this pressure. In many people, however, the veins’ valves stop working. We are not sure exactly why this happens. But many risk factors for developing venous insufficiency work together to contribute to the appearance of varicose veins, spider veins, and other symptoms of vein disorders.
Venous insufficiency symptoms
When vein valves stop working correctly, they leak blood back towards the feet, resulting in increased pressure. This often causes symptoms like swelling and aching initially. If it persists, the branches of the veins start enlarging and becoming more visible in the leg. This can result in one or more of these visible symptoms:
- Small spider-like veins called “spider veins” or “telangectasias”
- Medium sized veins (2-3 mm) called “reticular veins“
- Larger ropy veins called “varicose veins“
- Serious venous disease that results in sores on the legs called leg ulcers.
Risk Factors and Causes
The likelihood of developing varicose veins, spider veins or other symptoms of vein disorder is based on a variety risk factors or causes. Some risk factors are controllable like lifestyle and obesity. Other risk factors are not controllable such as genetics. If you have one or more of these varicose vein risk factors, you are at increased risk of developing spider veins or varicose veins.
- Genetics: Did your mother and grandmother have varicose veins? Do any of your siblings? Then, there is a fairly good chance that you may develop varicose veins as well. Not all cases of genetic predisposition develop varicose veins, but venous disorder does run in families.
- Age: As we get older, the elasticity in our vein walls decreases. This increases the possibility that valves will fail and varicose veins will develop.
- Gender: Females are much more likely to develop spider or varicose veins (although 25% of cases occur in males). Some research indicates increased levels of female hormones may cause relaxation of vein walls and may lead to valve failure.
- Pregnancy: The enlarged uterus during pregnancy can cause increased pressure on all veins. Combined with elevated hormone levels and heavier weight, pregnant women are at higher risk for varicose veins. This is typically for the first time while pregnant or shortly thereafter. Venous insufficiency usually gets worse with subsequent pregnancies and may improve somewhat after childbirth when the uterus, hormones, and weight return to normal.
- Lifestyle: People whose occupations require them to stand or sit for long periods of time are at higher risk. Professions like waitresses, hairdressers, and office workers, are statistically more likely to develop varicose veins.
- Obesity: Weight gain or carrying excessive body weight increases the risk for varicose veins and venous insufficiency. This may be because of increased pressure on the venous system in obese individuals. It may also be because of the disruption of the geometry of the valves in the tissues. Often, losing weight helps alleviate the symptoms of damagedveins in obese patients. Diet can have an effect as well.
- Injury: Trauma may injure veins and cause valves to fail, leading to symptoms of venous insufficiency. Examples of trauma includes a broken leg, knee, or hip surgery. Even a blunt injury that doesn’t involve broken bones such as an auto accident can increase risk. It is important to share any history of trauma with your physician so that proper diagnosis and treatment can be determined.
Diagnosing Venous Insufficiency or Varicose Veins
When diagnosing varicose veins or spider veins it is important to know the root cause of the problem. Essentially vein disease affects the ability of the body to circulate blood effectively. It happens when valves in the veins become weakened or fail. The venous system then has trouble preventing blood from pooling or flowing backwards as the body tries to pump blood against gravity and back to the heart. When this happens, it is considered vein disease or venous insufficiency. In order to diagnose varicose veins you must first determine if there is venous insufficiency.
Ultrasound for diagnosing venous insufficiency
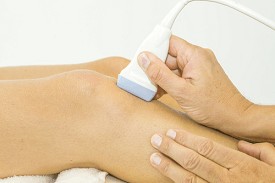
Ultrasound for diagnosing deep vein thrombosis
Ultrasound can also be an invaluable tool as it can tell us if there are blood clots in the veins. These can be potentially dangerous because they can lead to a serious condition called deep vein thrombosis.
Diagnosis leads to treatment
If you have varicose veins or signs of venous insufficiency, you should have an ultrasound as part of your evaluation. The ultrasound is painless and takes 30-45 minutes. At the San Francisco Vein Center, our experienced vascular ultrasound technologists make it possible to diagnose the underlying problems causing our patients’ varicose veins. Once we see which veins aren’t working correctly, we are able to formulate a treatment strategy customized to each patient.
Treating venous disorders
It is important to realize that varicose veins, spider veins, and reticular veins typically happen for a reason reason. They happen because veins in the lower leg are functioning poorly and may need to be treated. Varicose veins, spider veins, and venous ulcers are all evidence of venous insufficiency in the legs or other areas of the body. Treating venous insufficiency is the only way to mitigate future damage as well as to lessen uncomfortable symptoms and the unsightly appearance. To treat venous disorder in legs, vascular surgeons may use a variety of solutions depending on the patient’s particular needs:
- compression stockings
- radiofrequency ablation
- sclerotherapy
- stab phlebectomy
- traditional endovascular surgery
Only a board certified vascular surgeon like Dr. Aquino has all these options available.