MESENTERIC ISCHEMIA
What is Mesenteric Ischemia?
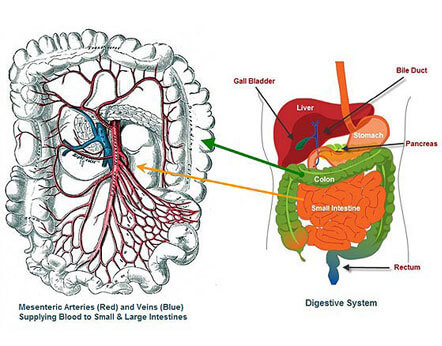 Mesenteric ischemia occurs when atherosclerosis (hardening of the arteries) happens in the blood vessels that supply blood to the intestines. This generally occurs in patients who already have fairly extensive peripheral vascular disease and atherosclerosis.
Mesenteric ischemia occurs when atherosclerosis (hardening of the arteries) happens in the blood vessels that supply blood to the intestines. This generally occurs in patients who already have fairly extensive peripheral vascular disease and atherosclerosis.
Risks and causes
Patients with mesenteric ischemia typically have a history of smoking. They often have had problems with atherosclerosis in the past such as heart attacks, claudication, etc
Symptoms
Because of the narrowing of the blood vessels leading to the intestines, people with this condition often have severe abdominal pain after eating. After eating, the intestine requires more blood to digest food and the narrowed arteries cannot supply the blood needed to the intestines. This deficiency results in pain. Patients with mesenteric ischemia usually start eating less because of pain and can come to the attention of a vein doctor after a considerable weight loss.
Diagnosis
Mesenteric ischemia is diagnosed in a few different ways. It is most commonly diagnosed with either an ultrasound or a CT scan. The ultrasound can diagnose narrowings in the blood vessels leading to the intestines by measuring the flow patterns and velocities of the blood. CT scans are useful because they show a direct picture of the narrowed blood vessels.
Treatment
Mesenteric artery stenosis and mesenteric ischemia is most often treated with endovascular stenting. This is a minimally invasive technique which usually involves a small puncture in an artery in the arm or groin. The vascular surgeon then is able to carefully direct a stent into the precise area where the artery narrows. The stent expands using a balloon. The balloon is withdrawn, leaving the stent in place. In this way, blood flows more easily into the arteries of the intestines and the patient often experiences dramatic relief of their symptoms.
